There is something quietly extraordinary about looking inside a living body without making a single incision. Radiology makes that possible. It sits at the heart of modern medicine — not merely as a diagnostic tool, but as a discipline that shapes clinical decisions, guides surgical planning, and often determines whether a patient walks out of a hospital in weeks or in months. For doctors and healthcare providers working in the UK or across the Gulf, understanding the full scope of contemporary radiology is foundational.
What Radiology Actually Encompasses
Radiology uses imaging technology — from conventional X-rays and ultrasound to MRI, CT, nuclear medicine, and interventional procedures — to diagnose and treat disease. The radiologist functions as both interpreter and, increasingly, as an active participant in treatment through image-guided interventions.
Diagnostic radiology covers musculoskeletal, neuroradiology, breast imaging, cardiovascular imaging, paediatric radiology, and emergency radiology. Interventional radiology uses real-time imaging to perform minimally invasive procedures: arterial embolisation, tumour ablation, image-guided biopsy, and central venous access. Together, these branches touch nearly every clinical discipline in the hospital.
Core Imaging Modalities and Their Clinical Applications
X-ray radiography remains the workhorse of emergency departments worldwide — fast, accessible, and relatively low-dose. CT delivers cross-sectional anatomical detail that plain radiography cannot match, enabling detection of pulmonary emboli, aortic dissection, and solid organ injury with sensitivity that has transformed trauma care.
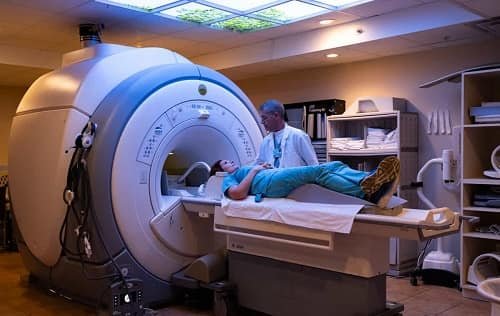
MRI offers unparalleled soft-tissue contrast without ionising radiation. Neurosurgeons rely on it for pre-operative planning; orthopaedic surgeons use it for ligamentous injury characterisation; oncologists request whole-body diffusion-weighted sequences for staging. Ultrasound places real-time imaging at the point of care, while PET-CT completes the toolkit by showing not just where a lesion sits, but how it behaves physiologically — detecting metabolically active deposits that standard CT might miss entirely.
Interventional Radiology: Where Imaging Becomes Treatment
The growth of interventional radiology represents one of the most significant developments in modern surgery. Transarterial chemoembolisation and radiofrequency ablation extend survival in hepatocellular carcinoma patients who are not surgical candidates. Endovascular aortic repair has transformed aneurysm management. Uterine fibroid embolisation offers a uterus-preserving alternative to hysterectomy. Each procedure demands technical precision alongside deep knowledge of cross-sectional anatomy, contrast pharmacology, and radiation safety.
Radiology in a Global Context: The UAE Experience
Healthcare infrastructure across the Gulf has expanded rapidly. For clinicians exploring radiology in Dubai, the standard of practice has risen considerably to meet international benchmarks. JCI-accredited facilities now operate imaging departments equipped with 3-Tesla MRI systems, 128-slice CT scanners, and fully digital fluoroscopy suites — all governed by radiation protection standards consistent with IAEA guidelines.
Dubai’s patient population spans over 200 nationalities, creating unique diagnostic demands. Radiologists must maintain familiarity with hepatocellular carcinoma in hepatitis-B-endemic populations, tuberculosis reactivation, haemoglobinopathies, and the full spectrum of metabolic syndrome sequelae — an environment both demanding and genuinely enriching for any specialist committed to developing diagnostic acuity.
Radiation Safety and Artificial Intelligence
Every clinician requesting imaging shares the responsibility for radiation safety. The “As Low As Reasonably Achievable” (ALARA) principle is the foundation for all ionising radiation use. In the UK, the IR(ME)R 2017 provides a clear legal framework: referrers must justify why the scan is needed, practitioners must ensure the technique is optimised, and operators must follow specific protocols during the procedure.
Special care is vital in paediatric cases. Because children are more sensitive to radiation, we should always consider whether a different type of scan—one that doesn’t use radiation—could be used instead. Algorithms struggle with rare conditions, unusual presentations, and the clinical context that an experienced radiologist brings instinctively to every reporting session. The radiologist who understands these tools’ strengths and integrates their outputs intelligently will remain indispensable.
Choosing the Right Facility
A well-functioning radiology department offers more than up-to-date equipment. It provides subspecialty reporting, MDT integration, and rapid turnaround on urgent cases. Patients requiring comprehensive diagnostic evaluation benefit most from the best multispeciality hospital Dubai has to offer — where radiological findings feed directly into surgical, oncological, and medical management, producing far more clinically useful reports than those generated in isolation.
Conclusion
Radiology sees the unseeable, guides the surgeon’s hand, and increasingly predicts outcomes before symptoms fully declare themselves. For clinicians across the UK and UAE, demanding the highest standards from imaging services remains one of the most direct levers available for improving patient outcomes. Technology evolves constantly. The clinical imperative does not.